Abstract
Risk stratification and population health analysis are integral to any health plan’s operations. When these tools are successfully used and implemented, organizations can more efficiently focus their resources, improve member health, and reduce costs.
Plenty of analytics vendors already exist. They often provide massive lists of members ranked by a handful of data points, mostly from claims. However, they’re unlikely to:
• Factor in social determinants of health (SDOH) or health-related social needs (HRSN)
• Employ strategies to mitigate potential algorithmic bias
• Tell the user what they can actually do to help any given member improve their health
Tools like these may work fine for the big commercial plans, their big analytics teams, and their even bigger budgets. But for small-to-midsize plans with fewer resources, the results lack the granularity necessary to design meaningful—and feasible—initiatives.
THE PROBLEM
Mountain Health CO-OP (the CO-OP) is one of the few remaining ACA-era CO-OPs and a community health plan providing essential coverage for a large, rural 3-state region. It has prevailed by being innovative and using proactive strategies to improve and maintain member health. For example, the organization fully covers insulin for members with diabetes. This helps prevent medication rationing and the costly consequences of untreated diabetes among members with a lower income.
Despite having a traditional predictive analytics tool and HEDIS vendor in place, the CO-OP had a number of questions that existing solutions could not answer, limiting their ability to address their members’ needs in the maximal way they envisioned. For example:
- Membership was growing, but churn needed to be minimized. How could they increase member retention and strengthen their long-term relationships with members?
- With known transportation and access barriers, how could they prioritize outreach and interventions around the members who needed it most?
- How could they adjust for risk and receive the resources needed to cover the complex populations they serve?
- How could they close quality gaps, improve their HEDIS score, and thereby support member wellbeing?
Furthermore, with competing priorities, how might they find these answers using existing datasets?
With their existing predictive analytics vendor, the CO-OP received large lists of members at high, medium, and low risk of predicted cost increases. The results were broad and provided limited rationale or information about SDOH, HRSN, or bias mitigation. The tool also did not provide specific interventions or insights that could be used to impact these risk trajectories.
They didn’t need a “bigger list” of high-risk members. They needed a “better list,” one that tied members to specific CO-OP-driven initiatives that could meaningfully impact them.
The Solution
These unanswered questions led the CO-OP to partner with Siftwell. Siftwell’s models are AI-powered and trained specifically on each client, making outputs richer, more comprehensive, and more intuitive. We knew the CO-OP needed to prioritize their outreach and interventions toward the people who would benefit most—and that those interventions had to be right the first time around.
“We don’t have a lot of do-overs as a CO-OP plan,” shared Blair Fjeseth, Chief Operating Officer at Mountain Health CO-OP.
Siftwell’s work centered around augmenting the CO-OP’s data with SDOH and HRSN datasets to enable a more granular view of which members were at risk for certain outcomes over the next year, and why. These outcomes included:
- Voluntary disenrollment from the plan
- Non-participation in health care due to solvable barriers such as transportation
- Development of novel comorbidities, at both the diagnosis and condition category (CC) level
- Non-compliance with needed screenings, including breast, colorectal, and cervical cancer screenings
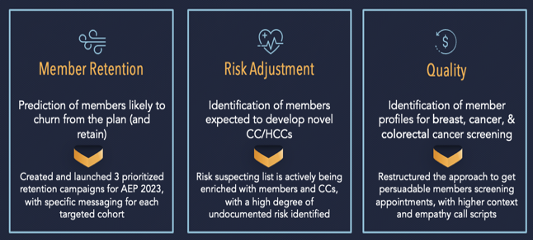
Siftwell’s solution enabled the CO-OP with membership insights, but most importantly enabled tangible action planning that is already yielding results. The CO-OP’s questions are significant ones that take consistent and determined effort to answer.
But in the short time of working together, the CO-OP has already realized demonstrable membership growth and retention, as well as increased outbound call answer rates for cancer screenings. Ripple effects of Siftwell’s work have also included reduced workload on staff, more pointed goals and tasks for teams to organize around, increased staff retention, decreased overall burnout, and a newfound joy for understanding their members at a deep level and being able to empathetically engage them.
“Siftwell brings to the table the latest in AI know-how and marries that with the community health plan context we live in,” said Fjeseth.
Your Partner in Improving Outcomes
Through the precision of AI, built-in considerations of SDOH and HRSN, and an ongoing collaboration with our data scientists, the CO-OP can now more easily move the needle on all its priorities. Whether they’re aiming to reduce member churn, adjust for emerging risk cases, boost their HEDIS score, or inform any other initiative, Siftwell will be with them every step of the way.
Ready to experience the Siftwell difference? Send us your data as is, tell us your goals, and we’ll get to work finding solutions that make sense for you.
Choosing Siftwell: The Rationale
Why did the CO-OP partner with Siftwell? What made Siftwell’s approach different from traditional tools used by the commercial plans?
Shared History, Shared Values
In a few words: Siftwell has been the CO-OP. Our founders have lived through the unique challenges of managing risk in the public, nonprofit sector. Accordingly, Siftwell’s entire approach is built from the ground up to alleviate the client’s workload, provide clarity, and deliver practical, timely solutions to their most pressing concerns. Our model was built precisely for plans like the CO-OP.
Explainable AI = Accuracy, Granularity, Transparency & Actionability
Siftwell’s artificial intelligence (AI) models are powerful tools to optimize the existing resources of a smaller health plan.
First, Siftwell identifies the high-risk members that other tools miss. Unlike traditional risk stratification methods, Siftwell feeds data into its algorithms and asks them to answer a question based on the thousands (or millions) of complex interactions between data points in the dataset.
The “machine” determines the association between these variables, which substantially improves accuracy and surfaces patterns often invisible to the human eye. Clinicians and health plan operators then review the outputs to ensure the findings are correct and representative.
Because of this, Siftwell’s insights are more accurate, granular, and precise. When we first engaged with the CO-OP, Siftwell ran its models against their existing tool for validation. Below, we share some of the most notable findings (also shown in the figure below):
- Siftwell’s models found that high-risk members were bound to cost more than double other tools’ predictions.
- Siftwell’s models also identified high-risk members the other tools missed. Our algorithms discovered that 47% of members classified by the existing tool as “Moderate Risk” by the prior tool were actually High or Very High risk.
- These members were more likely to suffer from neurologic disorders, mental health issues, and live in small towns, among other factors.
Uniquely, Siftwell’s model further segments these higher-risk member cohorts into Member Profiles. This allowed the CO-OP to understand at the “micro-cohort” level 1) who these members were and 2) what was driving their increased risk trajectory across clinical, social, and other factors.
From this actionable data, the CO-OP could decide how to best intervene and track intervention progress longitudinally. Siftwell’s team of data scientists and managed care operators worked alongside the CO-OP as needed to interpret results and augment strategy development.
Ethical Considerations
It was important to the CO-OP that any AI-driven initiative was built ethically and with special attention to potential bias.
Siftwell, since its conception, has understood the risk of bias in both data analytics and the broader healthcare system. Unmitigated bias can skew data outputs and damage health equity efforts. Knowing this, we employ an array of techniques when collecting and aggregating predictive models, such as:
- Comparing emerging-risk cohorts to “data twins” (people who share socio-economic identifiers) to help control for variables that may be impacted by societal bias
- Collecting diverse data sources to train our algorithm to also consider health-related social needs (not just claims data, which is disproportionately available for certain demographic groups)
- Building features to ensure certain demographic groups are not over-indexed in predicted results, so humans can review and adjust the outcome
Tailored Approach
Siftwell’s approach allows our models to answer partnering clients’ specific questions, as opposed to clients needing to pick and choose which of our models to use. For every health plan, we train our models so they reflect the nuance of their unique population. Then, based on backtesting results, we choose only the best performing models to generate final priority Member Profiles.
The CO-OP wanted to reduce member churn, improve quality, and adjust for risk. We tailored our models to address these concerns and suggest clear, actionable interventions.
Action Orientation
Siftwell considers its job “done” when members are impacted. Providing insights is just the first step, the base of the pyramid, in making that impact. Everything we do is intended to make it as easy as possible for our community-based clients to do what they do best – relate to their communities. And we stand by their side every step of the way.
*Click the download arrow below to download a shareable case study 1-sheet


